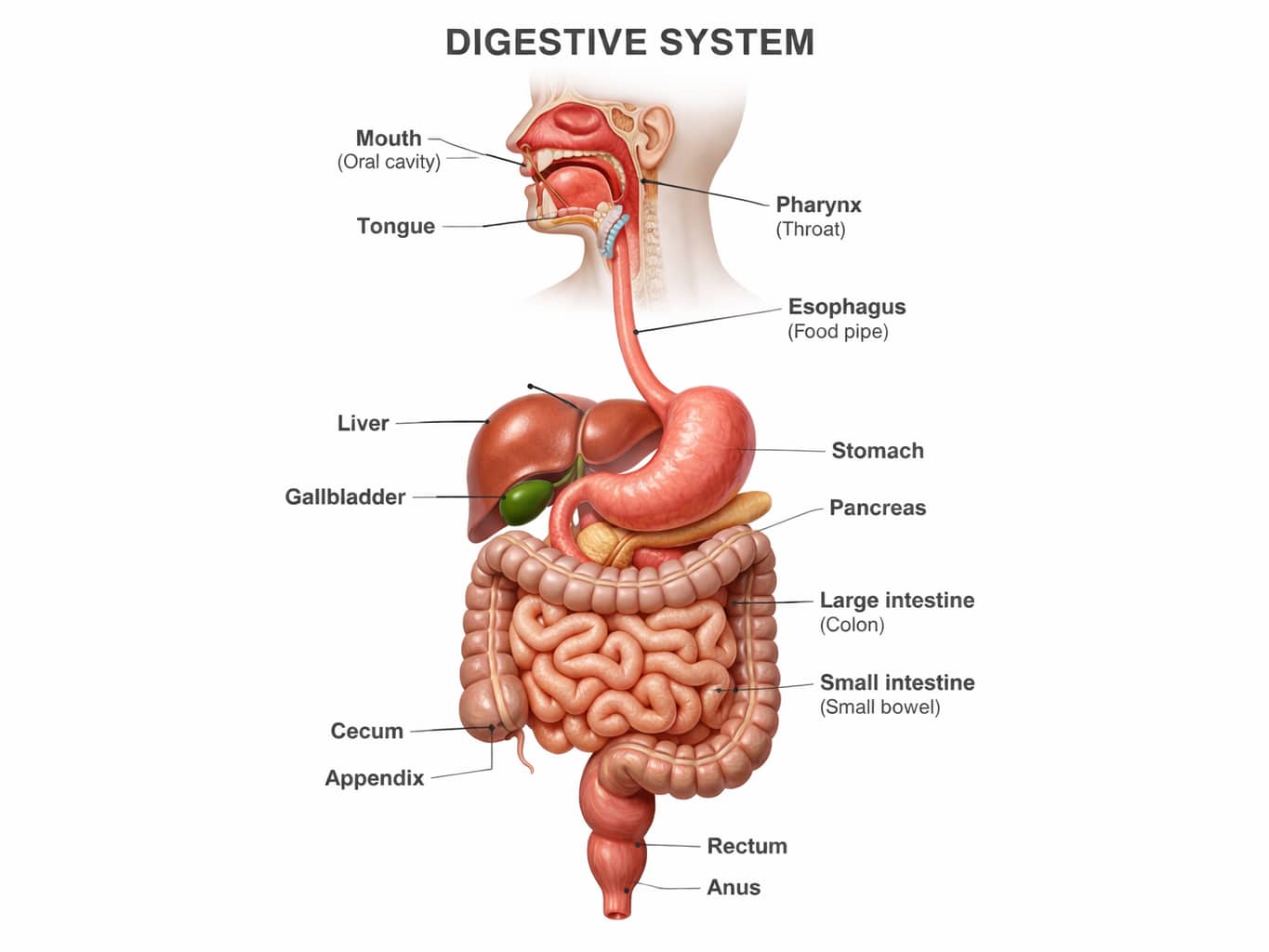
Stomach and intestinal problems are rarely just about what we eat. It is often about how the body handles food and whether the protective systems that keep the intestines in balance are working properly.
Two conditions that are often linked are SIBO (Small Intestinal Bacterial Overgrowth) and leaky gut. They are sometimes described as separate problems, but in practice they are often different expressions of the same underlying imbalance.
SIBO – a functional problem, not just a bacterial problem
SIBO means there are too many bacteria in the small intestine, where bacterial levels should normally be relatively low. These bacteria begin to ferment food, which can cause bloating, gas, and nutritional deficiencies.
It is often described as bacteria from the large intestine migrating upwards, but the picture is more complex. Bacteria are continuously introduced via both the oral cavity and food and are under normal conditions effectively handled by stomach acid, enzymes and bile. SIBO occurs when this control fails.
For the small intestine to function optimally, an interaction between several functions is required. Stomach acid acts as a first line of defense against microorganisms, and when stomach acid is low, more bacteria survive and can move further down the system.
The motility of the intestine, its ability to move, is crucial. Between meals, a cleaning program is activated that removes bacteria and residues. If this does not work, for example during stress, sedentary lifestyle or snacking, stagnation occurs.
Bile plays a central, but often underestimated, role. In addition to its function in fat digestion, bile acids have a direct antimicrobial effect and help regulate both the intestinal environment and motility. When bile flow is reduced, this control is reduced, which can create a more stagnant environment where bacteria can more easily gain a foothold.
At the same time, the overgrowth leads to an increased amount of bacterial components such as LPS (lipopolysaccharides). Inflammatory substances from the cell wall of some bacteria that are released when bacteria break down, which can increase inflammation. Reduced enzyme production also means that food is not broken down properly, which gives bacteria more raw material to ferment.
Another factor is the ileocecal valve, the structure that separates the small intestine from the large intestine. When it is impaired, such as in cases of stagnation, constipation, or increased pressure in the abdomen, bacteria from the large intestine can more easily enter the small intestine and contribute to overgrowth.
What these factors have in common is that they create an environment where digestion is slow and incomplete, which provides a perfect breeding ground for overgrowth.

Leaky gut – when the barrier starts to let through
The lining of the intestine acts as a selective barrier. It is designed to let nutrients through, but keep bacteria, toxins and larger molecules out. When this barrier weakens and becomes more permeable, what is often called leaky gut occurs.
This is an actively regulated process in which the protein zonulin plays a central role. Zonulin acts as an opening mechanism between the cells in the intestinal mucosa. When levels increase, the so-called tight junctions, the structures that hold the cells tightly together and act as a barrier, open, allowing more to pass through than is optimal.
Several factors can drive this process. One of the most studied is gluten, especially the component gliadin. Gliadin can both stimulate the release of zonulin and directly irritate the intestinal mucosa. This is clear in celiac disease, but the same mechanism can be activated to varying degrees even in people without a diagnosed disease. In an already burdened intestine, for example in SIBO, this effect can be more pronounced.
At the same time, SIBO contributes to further strain on the barrier. The overgrowth in the small intestine means an increased amount of bacterial byproducts, including LPS, which drive inflammation and can negatively affect both the intestinal mucosa and tight junctions.
When the barrier weakens, substances that are normally retained in the intestine can pass into the bloodstream. This triggers the immune system and contributes to low-grade, systemic inflammation.
Leaky brain and autoimmunity
The intestinal barrier is not only a physical boundary, but also a central part of the immune system’s regulation. Here the body is trained to distinguish between what is native to the body, what is harmless, and what is a threat.
When permeability increases, the immune system is exposed to substances it should not normally encounter, such as incompletely broken down proteins, gliadin, or bacterial components such as LPS.
One mechanism that is being discussed is so-called molecular mimicry, where structures in these substances resemble the body’s own tissues. When the immune system is activated, the reaction can in some cases also be directed against the body itself.
This does not mean that leaky gut itself causes autoimmune disease, but it may be a contributing factor in a larger context where genetics, environment and lifestyle interact.
These same inflammatory signals can also affect other barriers in the body, not least the blood-brain barrier. When this is affected, it can contribute to symptoms such as brain fog, fatigue and cognitive impairment. Sometimes described as a form of “leaky brain.”
What can you do yourself?
Since the problem is fundamentally about function, that is also where the solution begins.
- Creating clear meal intervals, where there are approximately 3–4 hours between meals, gives the intestines the opportunity to activate their cleaning system and reduce stagnation.
- Eating in a calm environment and chewing your food thoroughly supports stomach acid and enzyme production. Stress has the opposite effect and is therefore a key factor to work with.
- Bitter foods like apple cider vinegar, arugula, and endive can stimulate both stomach acid and bile flow.
- Regular exercise, especially walking, improves intestinal motility.
- Avoid drinking large amounts of fluid immediately after meals – instead hydrate between meals.
- Avoid intestinal irritants, such as gluten, especially if your intestines are already stressed.
For more pronounced symptoms, a temporary dietary intervention may be helpful, such as a low-FODMAP or a strict animal-based diet (carnivore). These reduce the amount of fermentable substrate and can thus alleviate symptoms.
With a carnivore diet, it is especially important to simultaneously support stomach acid and digestion. Otherwise, there is a risk that protein breakdown will be impaired and new imbalances will arise later on. This type of diet is therefore not a long-term solution, but a temporary intervention to calm the system and reduce the bacterial load.
At the same time, the root cause always needs to be addressed. If low stomach acid, impaired motility, bile problems or a failing ileocecal valve persist, the risk of recurrence is high.
For those who want to do a more in-depth investigation, it may be valuable to work with a therapist or doctor who focuses on restoring balance to the digestive system. There are also medical treatment options, such as antibiotics, but even there it is crucial that the underlying causes are addressed.
Ultimately, SIBO and leaky gut are not primarily about eliminating bacteria, but about restoring the body’s function. When digestion is working, when bowel movements are intact, and when the barrier is strong, the body itself creates an environment where overgrowth does not take hold. It is only when this balance is disturbed that problems arise and that is also where the road back begins.
References
-
Achufusi TO et al. Small Intestinal Bacterial Overgrowth: Comprehensive Review of Diagnosis, Prevention, and Treatment Methods. Cureus, 2020. https://pubmed.ncbi.nlm.nih.gov/32754400/
-
Camilleri M. The Leaky Gut: Mechanisms, Measurement and Clinical Implications in Humans. Gut, 2019. https://pmc.ncbi.nlm.nih.gov/articles/PMC6790068/
-
Martin et al. A Zero Carbohydrate, Carnivore Diet can Normalize Hydrogen Positive Small Intestinal Bacterial Overgrowth Lactulose Breath Tests: A Case Report, 2021 https://www.researchsquare.com/article/rs-148500/v1